Scientists are warning about a potential increase in risk of waterborne infections, including Legionnaires’ disease1.
Legionnaires’ disease (LD) is a severe form of pneumonia contracted by inhaling droplets of contaminated water in the air (aerosols) or via aspiration of contaminated water. It mainly affects people > 50 years, current or former smokers, and those with chronic respiratory illnesses or weakened immune systems. Symptoms have similarities with a COVID-19 infection: cough, shortness of breath and fever, as well as muscle- and headache. A rise in Legionella cases was seen in the United States and Europe, who both now report rates of about 1.3-1.6 cases per 100,000 population2 with a mortality rate estimated of 5-15%3.
Learn more about current published guidelines on how to safely manage water distribution systems during the COVID-19 pandemic by filling out the form.
Learn more about the published guidelines

Thank you for filling out the form! The Pall Statement will be emailed to you shortly.
Can Legionella and COVID-19 be connected?
These two diseases are in fact markedly different: The pathogen causing COVID-19 is a virus transmitted through aerosols / surfaces, while Legionella are bacteria commonly found in water. But there are similarities and interconnections too:
- Both pathogens disproportionately affect the elderly and those with preexisting conditions, and both diseases affect the lungs. Legionella is thought to cause up to 9% of community-acquired pneumonia4.
- Many old buildings with old pipe systems, and hence a higher risk of Legionella contamination, are being repurposed as field hospitals to take care of COVID-19 patients – who as hospital in-patients have a higher mortality rate when also infected with Legionella5.
- Co- and secondary infections: With both influenza viruses and coronavirus, complications from secondary bacterial infections or co-infections can lead to a significant increase of morbidity and mortality. Bacterial co-infections are more common with viral infections because many viruses can suppress the host immune response, particularly in the elderly or those with chronic medical diseases. There have been cases of swine flu and pneumonia due to Legionella as well as respiratory failure in influenza patients after infection with Legionella6.
What does this mean for the current crisis?
In the coming weeks and months, hotels, schools, gyms, restaurants and other businesses will start to re-open and the water will be used for the first time in weeks or months in these buildings, if the recommended guidelines have not been followed. In this time, any Legionella spp. in the system could have multiplied, posing a risk for contaminations.
What do the experts say?
Public health experts across the globe have been quick to react, urging landlords to use caution when re-opening buildings if the facility has been vacated or underutilized for longer than a week. The idea is “to prevent Legionella outbreaks to a) protect people and b) protect already overstretched health systems”, says Molly Scanlon, leader of the coronavirus task force of the American Institute of Architects. The threat also applies to sprinkler systems and water cooling towers on commercial buildings; these corporations will “likely be aware of the issue of stagnant water. However, “smaller businesses might not”, warns Susanne Surman-Lee, one of the co-authors of the European Society of Clinical Microbiology and Infectious Diseases Guidance for Managing Legionella in Building Water Systems During the COVID-19 Pandemic. But the British microbiologist also adds: “It’s a worldwide problem; one that can be solved with precautions”7.
So, what can communities do?
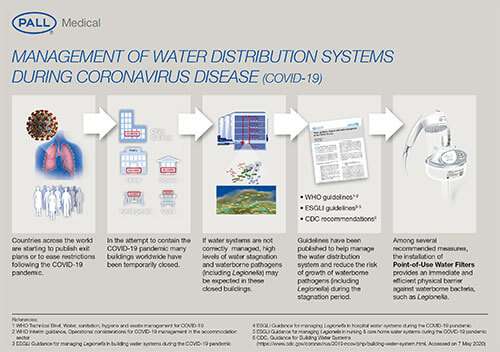
In the attempt to contain the COVID-19 pandemic many buildings worldwide, including: hotels, leisure centers, public buildings, schools, kindergartens, swimming pools, etc., have been temporarily closed and a high level of water stagnation is expected. As the experts advise, water stagnation can be an important contributing factor to the microbial growth within water installations, increasing the risk of Legionella and other waterborne pathogen contaminations. In addition, particular attention should be given to the water distribution systems of field hospitals and buildings (i.e. hotels, etc.), that have been repurposed as healthcare facilities to treat COVID-19 patients, to minimize the risk of coinfections8.
Therefore, international, regional and local guidelines have been published to help manage the water distribution system correctly and reduce the risk of growth of waterborne pathogens during stagnation periods. Besides flushing and maintaining the required temperatures for hot and cold water, chemical continuous or shock disinfection, emptying the water installation, the short-term installation of Point-of-Use Water Filters can provide an immediate and efficient physical barrier against waterborne bacteria and fungi.
References:
- ESCMID (2020). ESCMID Study Group for Legionella Infections – ESGLI. [online]. Available at: https://www.escmid.org/research_projects/study_groups/legionella_infections/ [Accessed 29 April. 2020].
- Beauté, J. (2017). The European Legionnaires' Disease Surveillance Network. Legionnaires' disease in Europe, 2011 to 2015.Euro Surveill. 2017;22(27), 1-8
- Brady M.F. et al. (2019) Legionnaires' Disease (Legionella Infection), StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan.
- Bradley, B.T. et al. (2019). Emerging respiratory infections: The infectious disease pathology of SARS, MERS, pandemic influenza, and Legionella. Semin Diagn Pathol, 36 (3): 152–159.
- Skerrett, SJ. (2018). Prevention of Health Care–Associated Legionnaires Disease. JAMA Network Open, 1 (2), 1-3
- Lin S.Y. et al. (2016). An Underestimated Co-infection: Swine Influenza and Pneumonia Due to Legionella pneumophila, Am J Med Sci,352(3):314-316
- Reuters (2020). Buildings closed by coronavirus face another risk: Legionnaires’ disease. [online]. Available at: https://www.reuters.com/article/health-coronavirus-legionnaires-idUSL3N2CB4VZ [Accessed 29 April. 2020].
- Xing, Q. et al. (2020). Precautions are Needed for COVID-19 Patients with Coinfection of Common Respiratory Pathogens medRxiv 2020.02.29.20027698; doi: https://doi.org/10.1101/2020.02.29.20027698